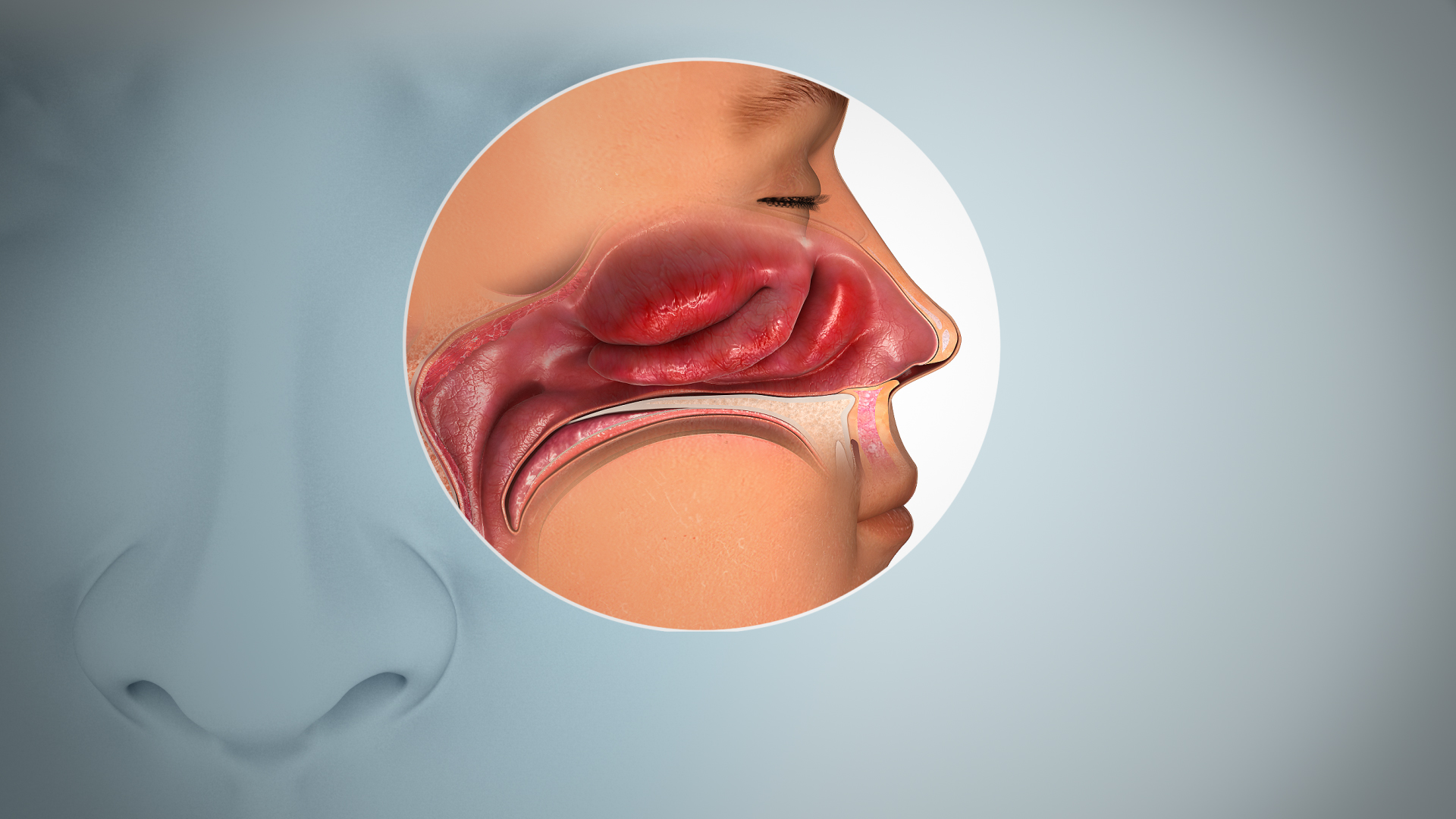
Anosmia
Anosmia can be due to a number of factors, including inflammation of the nasal mucosa, blockage of nasal passages, or destruction of temporal lobular tissue.[4] Anosmia stemming from sinus inflammation is due to chronic mucosal changes in the lining of the paranasal sinus and in the middle and superior turbinates.[5][6]
When anosmia is caused by inflammatory changes in the nasal passageways, it is treated simply by reducing inflammation.[7][8] It can be caused by chronic meningitis and neurosyphilis that would increase intracranial pressure over a long period of time,[9] and, in some cases, by ciliopathy,[10] including ciliopathy due to primary ciliary dyskinesia.[11]
The term derives from the Neo-Latin anosmia, based on Ancient Greek ἀν- (an-) + ὀσμή (osmḗ 'smell'; another related term, hyperosmia, refers to an increased ability to smell). Some people may be anosmic for one particular odor, a condition known as "specific anosmia". The absence of the sense of smell from birth is known as congenital anosmia.[12]
In the United States, 3% of people aged over 40 are affected by anosmia.[3]
Anosmia is a common symptom of COVID-19 and can persist as long COVID.[13]
Signs and symptoms[edit]
Anosmia can have a number of harmful effects.[14] People with sudden onset anosmia may find food less appetizing, though congenital anosmics rarely complain about this, and none report a loss in weight. Loss of smell can also be dangerous because it hinders the detection of gas leaks, fire, and spoiled food. Misconceptions of anosmia as trivial can make it more difficult for a patient to receive the same types of medical aid as someone who has lost other senses, such as hearing or sight.
Many experience one sided loss of smell, often as a result of minor head trauma. This type of anosmia is normally only detected if both of the nostrils are tested separately. Using this method of testing each nostril separately will often show a reduced or even completely absent sense of smell in either one nostril or both, something which is often not revealed if both nostrils are simultaneously tested.[15]
Losing an established and sentimental smell memory (e.g. the smell of grass, of the grandparents' attic, of a particular book, of loved ones, or of oneself) has been known to cause feelings of depression.[16]
Loss of the ability to smell may lead to the loss of libido, but this usually does not apply to those with olfactory dysfunction at birth.[16][17]
Often people who have loss of smell at birth report that they pretended to be able to smell as children because they thought that smelling was something that older/mature people could do, or did not understand the concept of smelling but did not want to appear different from others. When children get older, they often realize and report to their parents that they do not actually possess a sense of smell, often to the surprise of their parents.
Diagnosis[edit]
Diagnosis begins with a detailed history, including possible related injuries, such as upper respiratory infections or head injury. The examination may involve nasal endoscopy for obstructive factors such as polyps or swelling.[4] A nervous system examination is performed to see if the cranial nerves are affected.[4] On occasion, after head traumas, there are people who have unilateral anosmia. The sense of smell should be tested individually in each nostril.[15]
Many cases of congenital anosmia remain unreported and undiagnosed. Since the disorder is present from birth the individual may have little or no understanding of the sense of smell, hence is unaware of the deficit.[51] It may also lead to reduction of appetite.[52]
Treatment[edit]
Though anosmia caused by brain damage cannot be treated, anosmia caused by inflammatory changes in the mucosa may be treated with glucocorticoids. Reduction of inflammation through the use of oral glucocorticoids such as prednisone, followed by long term topical glucocorticoid nasal spray, would easily and safely treat the anosmia. A prednisone regimen is adjusted based on the degree of the thickness of mucosa, the discharge of oedema and the presence or absence of nasal polyps.[7] However, the treatment is not permanent and may have to be repeated after a short while.[7] Together with medication, pressure of the upper area of the nose must be mitigated through aeration and drainage.[53]
Anosmia caused by a nasal polyp may be treated by steroidal treatment or removal of the polyp.[54]
Although very early in development, gene therapy has restored a sense of smell in mice with congenital anosmia when caused by ciliopathy. In this case, a genetic condition had affected cilia in their bodies which normally enabled them to detect air-borne chemicals, and an adenovirus was used to implant a working version of the IFT88 gene into defective cells in the nose, which restored the cilia and allowed a sense of smell.[55][56]
Epidemiology[edit]
In the United States 3% of people aged over 40 are affected by anosmia.[3]
In 2012, smell was assessed in persons aged 40 years and older with rates of anosmia/severe hyposmia of 0.3% at age 40–49 rising to 14.1% at age 80+. Rates of hyposmia were much higher: 3.7% at age 40–49 and 25.9% at 80+.[57]