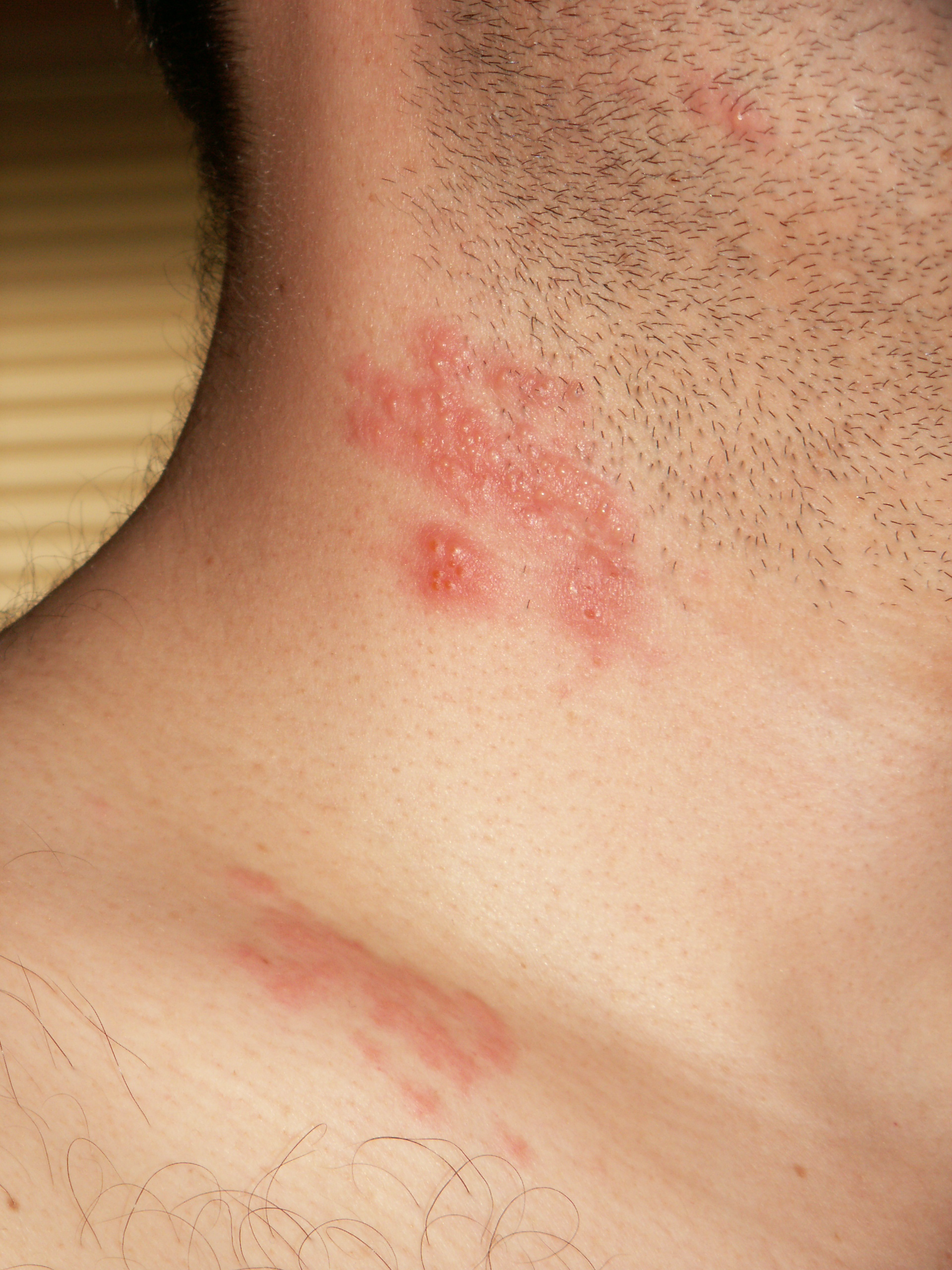
Shingles
Shingles, also known as herpes zoster, is a viral disease characterized by a painful skin rash with blisters in a localized area.[2][6] Typically the rash occurs in a single, wide mark either on the left or right side of the body or face.[1] Two to four days before the rash occurs there may be tingling or local pain in the area.[1][7] Other common symptoms are fever, headache, and tiredness.[1][8] The rash usually heals within two to four weeks;[2] however, some people develop ongoing nerve pain which can last for months or years, a condition called postherpetic neuralgia (PHN).[1] In those with poor immune function the rash may occur widely.[1] If the rash involves the eye, vision loss may occur.[2][9]
For other uses, see Shingle (disambiguation).Shingles
Herpes zoster
Painful rash
2–4 weeks[2]
Old age, poor immune function, having had chickenpox before 18 months of age[1]
Based on symptoms[3]
Herpes simplex, chest pain, insect bites, cutaneous leishmaniasis[4]
33% (at some point)[1]
6,400 (with chickenpox)[5]
Shingles is caused by the varicella zoster virus (VZV) that also causes chickenpox. In the case of chickenpox, also called varicella, the initial infection with the virus typically occurs during childhood or adolescence.[1] Once the chickenpox has resolved, the virus can remain dormant (inactive) in human nerve cells (dorsal root ganglia or cranial nerves)[10] for years or decades, after which it may reactivate and travel along nerve bodies to nerve endings in the skin, producing blisters.[1][7] During an outbreak of shingles, exposure to the varicella virus found in shingles blisters can cause chickenpox in someone who has not yet had chickenpox, although that person will not suffer from shingles, at least on the first infection.[11] How the virus remains dormant in the body or subsequently re-activates is not well understood.[1][12]
The disease has been recognized since ancient times.[1] Risk factors for reactivation of the dormant virus include old age, poor immune function, and having contracted chickenpox before 18 months of age.[1] Diagnosis is typically based on the signs and symptoms presented.[3] Varicella zoster virus is not the same as herpes simplex virus, although they belong to the same family of herpesviruses.[13]
Shingles vaccines reduce the risk of shingles by 50 to 90%, depending on the vaccine used.[1][14] Vaccination also decreases rates of postherpetic neuralgia, and, if shingles occurs, its severity.[1] If shingles develops, antiviral medications such as aciclovir can reduce the severity and duration of disease if started within 72 hours of the appearance of the rash.[3] Evidence does not show a significant effect of antivirals or steroids on rates of postherpetic neuralgia.[15][16] Paracetamol, NSAIDs, or opioids may be used to help with acute pain.[3]
It is estimated that about a third of people develop shingles at some point in their lives.[1] While shingles is more common among older people, children may also get the disease.[13] According to the US National Institutes of Health, the number of new cases per year ranges from 1.2 to 3.4 per 1,000 person-years among healthy individuals to 3.9 to 11.8 per 1,000 person-years among those older than 65 years of age.[8][17] About half of those living to age 85 will have at least one attack, and fewer than 5% will have more than one attack.[1][18] Although symptoms can be severe, risk of death is very low: 0.28 to 0.69 deaths per million.[10]
The rash and pain usually subside within three to five weeks, but about one in five people develop a painful condition called postherpetic neuralgia, which is often difficult to manage. In some people, shingles can reactivate presenting as zoster sine herpete: pain radiating along the path of a single spinal nerve (a dermatomal distribution), but without an accompanying rash. This condition may involve complications that affect several levels of the nervous system and cause many cranial neuropathies, polyneuritis, myelitis, or aseptic meningitis. Other serious effects that may occur in some cases include partial facial paralysis (usually temporary), ear damage, or encephalitis.[28] Although initial infections with VZV during pregnancy, causing chickenpox, may lead to infection of the fetus and complications in the newborn, chronic infection or reactivation in shingles are not associated with fetal infection.[71][72]
There is a slightly increased risk of developing cancer after a shingles episode. However, the mechanism is unclear and mortality from cancer did not appear to increase as a direct result of the presence of the virus.[73] Instead, the increased risk may result from the immune suppression that allows the reactivation of the virus.[74]
Although shingles typically resolves within 3–5 weeks, certain complications may arise:
History[edit]
Shingles has a long recorded history, although historical accounts fail to distinguish the blistering caused by VZV and those caused by smallpox,[36] ergotism, and erysipelas. In the late 18th century William Heberden established a way to differentiate shingles and smallpox,[100] and in the late 19th century, shingles was differentiated from erysipelas. In 1831 Richard Bright hypothesized that the disease arose from the dorsal root ganglion, and an 1861 paper by Felix von Bärensprung confirmed this.[101]
Recognition that chickenpox and shingles were caused by the same virus came at the beginning of the 20th century. Physicians began to report that cases of shingles were often followed by chickenpox in younger people who lived with the person with shingles. The idea of an association between the two diseases gained strength when it was shown that lymph from a person with shingles could induce chickenpox in young volunteers. This was finally proved by the first isolation of the virus in cell cultures, by the Nobel laureate Thomas Huckle Weller, in 1953.[102] Some sources also attribute the first isolation of the herpes zoster virus to Evelyn Nicol.[103]
Until the 1940s the disease was considered benign, and serious complications were thought to be very rare.[104] However, by 1942, it was recognized that shingles was a more serious disease in adults than in children and that it increased in frequency with advancing age. Further studies during the 1950s on immunosuppressed individuals showed that the disease was not as benign as once thought, and the search for various therapeutic and preventive measures began.[105] By the mid-1960s, several studies identified the gradual reduction in cellular immunity in old age, observing that in a cohort of 1,000 people who lived to the age of 85, approximately 500 (i.e., 50%) would have at least one attack of shingles, and 10 (i.e., 1%) would have at least two attacks.[106]
In historical shingles studies, shingles incidence generally increased with age. However, in his 1965 paper, Hope-Simpson suggested that the "peculiar age distribution of zoster may in part reflect the frequency with which the different age groups encounter cases of varicella and because of the ensuing boost to their antibody protection have their attacks of zoster postponed".[22]
Lending support to this hypothesis that contact with children with chickenpox boosts adult cell-mediated immunity to help postpone or suppress shingles, a study by Thomas et al. reported that adults in households with children had lower rates of shingles than households without children.[107] Also, the study by Terada et al. indicated that pediatricians reflected incidence rates from 1/2 to 1/8 that of the general population their age.[108]
Etymology[edit]
The family name of all the herpesviruses derives from the Greek word έρπης herpēs,[109] from έρπω herpein ("to creep"),[110][111][112] referring to the latent, recurring infections typical of this group of viruses. Zoster comes from Greek ζωστήρ zōstēr,[113] meaning "belt" or "girdle", after the characteristic belt-like dermatomal rash.[114] The common name for the disease, shingles, derives from the Latin cingulus, a variant of Latin cingulum,[115] meaning "girdle".[116][117]
Research[edit]
Until the mid-1990s, infectious complications of the central nervous system (CNS) caused by VZV reactivation were regarded as rare. The presence of rash, as well as specific neurological symptoms, were required to diagnose a CNS infection caused by VZV. Since 2000, PCR testing has become more widely used, and the number of diagnosed cases of CNS infection has increased.[118]
Classic textbook descriptions state that VZV reactivation in the CNS is restricted to immunocompromised individuals and the elderly; however, studies have found that most participants are immunocompetent, and younger than 60 years old. Historically, vesicular rash was considered a characteristic finding, but studies have found that rash is only present in 45% of cases.[118]
In addition, systemic inflammation is not as reliable an indicator as previously thought: the mean level of C-reactive protein and mean white blood cell count are within the normal range in participants with VZV meningitis.[119]
MRI and CT scans are usually normal in cases of VZV reactivation in the CNS. CSF pleocytosis, previously thought to be a strong indicator of VZV encephalitis, was absent in half of a group of people diagnosed with VZV encephalitis by PCR.[118]
The frequency of CNS infections presented at the emergency room of a community hospital is not negligible, so a means of diagnosing cases is needed. PCR is not a foolproof method of diagnosis, but because so many other indicators have turned out to not be reliable in diagnosing VZV infections in the CNS, screening for VZV by PCR is recommended. Negative PCR does not rule out VZV involvement, but a positive PCR can be used for diagnosis, and appropriate treatment started (for example, antivirals can be prescribed rather than antibiotics).[118]
The introduction of DNA analysis techniques has shown some complications of varicella-zoster to be more common than previously thought. For example, sporadic meningoencephalitis (ME) caused by varicella-zoster was regarded as rare disease, mostly related to childhood chickenpox. However, meningoencephalitis caused by varicella-zoster is increasingly recognized as a predominant cause of ME among immunocompetent adults in non-epidemic circumstances.[120]
Diagnosis of complications of varicella-zoster, particularly in cases where the disease reactivates after years or decades of latency, is difficult. A rash (shingles) can be present or absent. Symptoms vary, and there is a significant overlap in symptoms with herpes-simplex symptoms.[120]
Although DNA analysis techniques such as polymerase chain reaction (PCR) can be used to look for DNA of herpesviruses in spinal fluid or blood, the results may be negative, even in cases where other definitive symptoms exist.[121] Notwithstanding these limitations, the use of PCR has resulted in an advance in the state of the art in our understanding of herpesviruses, including VZV, during the 1990s and 2000s. For example, in the past, clinicians believed that encephalitis was caused by herpes simplex and that people always died or developed serious long-term function problems. People were diagnosed at autopsy or by brain biopsy. Brain biopsy is not undertaken lightly: it is reserved only for serious cases that cannot be diagnosed by less invasive methods. For this reason, knowledge of these herpes virus conditions was limited to severe cases. DNA techniques have made it possible to diagnose "mild" cases, caused by VZV or HSV, in which the symptoms include fever, headache, and altered mental status. Mortality rates in treated people are decreasing.[120]