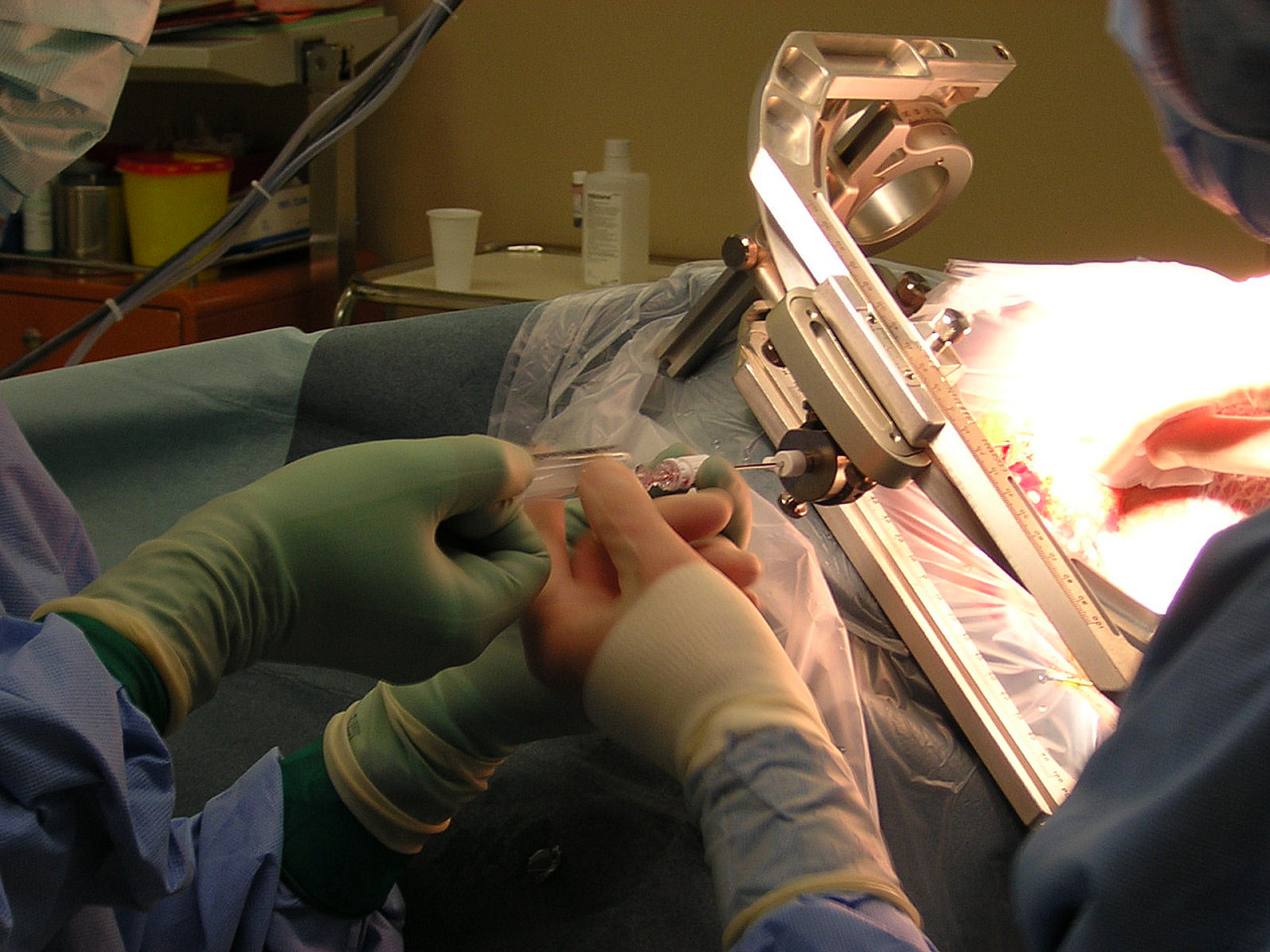
Stereotactic surgery
Stereotactic surgery is a minimally invasive form of surgical intervention that makes use of a three-dimensional coordinate system to locate small targets inside the body and to perform on them some action such as ablation, biopsy, lesion, injection, stimulation, implantation, radiosurgery (SRS), etc.
Not to be confused with the concept of stereotaxy in virtual reality.Stereotactic surgery
Stereotaxy
Neurosurgery
In theory, any organ system inside the body can be subjected to stereotactic surgery. However, difficulties in setting up a reliable frame of reference (such as bone landmarks, which bear a constant spatial relation to soft tissues) mean that its applications have been, traditionally and until recently, limited to brain surgery. Besides the brain, biopsy and surgery of the breast are done routinely to locate, sample (biopsy), and remove tissue. Plain X-ray images (radiographic mammography), computed tomography, and magnetic resonance imaging can be used to guide the procedure.
Another accepted form of "stereotactic" is "stereotaxic". The word roots are stereo-, a prefix derived from the Greek word στερεός (stereos, "solid"), and -taxis (a suffix of Neo-Latin and ISV, derived from Greek taxis, "arrangement", "order", from tassein, "to arrange").
Uses[edit]
The surgery is used to treat various brain cancers, benign, and functional disorders of the brain.[1] This is sometimes combined with whole brain radiotherapy, and a 2021 systematic review found this combination led to the greatest improvement of survival for those with single brain metastasis.[2]
Amongst the malignant brain disorders are: brain metastasis and glioblastoma.[1] The benign brain disorders are: meningioma, cerebral arteriovenous malformation, vestibular schwannoma, and pituitary adenoma.[1] Functional disorders are: trigeminal neuralgia, Parkinson's disease, and epilepsy.[1]
History[edit]
The stereotactic method was first published in 1908 by two British scientists, Victor Horsley, a physician and neurosurgeon, and Robert H. Clarke, a physiologist and was built by Swift & Son; the two scientists stopped collaborating after the 1908 publication. The Horsley–Clarke apparatus used a Cartesian (three-orthogonal axis) system. That device is in the Science Museum, London; a copy was brought to the US by Ernest Sachs and is in the Department of Neurosurgery at UCLA. Clarke used the original to do research that led to publications of primate and cat brain atlases. There is no evidence it was ever used in a human surgery.[28][29]: 12 [30] The first stereotactic device designed for the human brain appears to have been an adaptation of the Horseley–Clarke frame built at Aubrey T. Mussen's behest by a London workshop in 1918, but it received little attention and does not appear to have been used on people. It was a frame made of brass.[29]: 12 [31]
The first stereotactic device used in humans was used by Martin Kirschner, for a method to treat trigeminal neuralgia by inserting an electrode into the trigeminal nerve and ablating it. He published this in 1933.[29]: 13 [32]: 420 [33]
In 1947 and 1949, two neurosurgeons working at Temple University in Philadelphia, Ernest A. Spiegel (who had fled Austria when the Nazis took over[28]) and Henry T. Wycis, published their work on a device similar to the Horsley–Clarke apparatus in using a cartesian system; it was attached to the patient's head with a plaster cast instead of screws. Their device was the first to be used for brain surgery; they used it for psychosurgery. They also created the first atlas of the human brain, and used intracranial reference points, generated by using medical images acquired with contrast agents.[29]: 13 [32]: 72 [34]
The work of Spiegel and Wycis sparked enormous interest and research.[29]: 13 In Paris, Jean Talairach collaborated with Marcel David, Henri Hacaen, and Julian de Ajuriaguerra on a stereotactic device, publishing their first work in 1949 and eventually developing the Talairach coordinates.[28][29]: 13 [32]: 93 In Japan, Hirotaro Narabayashi was doing similar work.[28]
In 1949, Lars Leksell published a device that used polar coordinates instead of cartesian, and two years later he published work where he used his device to target a beam of radiation into a brain.[29]: 13 [32]: 91 [35][36] Leksell's radiosurgery system is also used by the Gamma Knife device, and by other neurosurgeons, using linear accelerators, proton beam therapy and neutron capture therapy. Lars Leksell went on to commercialize his inventions by founding Elekta in 1972.[37]
In 1979, Russell A. Brown proposed a device,[38] now known as the N-localizer,[39] that enables guidance of stereotactic surgery using tomographic images that are obtained via medical imaging technologies such as X-ray computed tomography (CT),[40] magnetic resonance imaging (MRI),[41] or positron emission tomography (PET).[42] The N-localizer comprises a diagonal rod that spans two vertical rods to form an N-shape that allows tomographic images to be mapped to physical space.[43] This device became almost universally adopted by the 1980s[44] and is included in the Brown-Roberts-Wells (BRW),[45] Kelly-Goerss,[46] Leksell,[47] Cosman-Roberts-Wells (CRW),[48] Micromar-ETM03B, FiMe-BlueFrame, Macom, and Adeor-Zeppelin[49] stereotactic frames and in the Gamma Knife radiosurgery system.[44] An alternative to the N-localizer is the Sturm-Pastyr localizer[50] that is included in the Riechert-Mundinger and Zamorano-Dujovny stereotactic frames.[51]
Other localization methods also exist that do not make use of tomographic images produced by CT, MRI, or PET, but instead conventional radiographs.[52]
The stereotactic method has continued to evolve, and at present employs an elaborate mixture of image-guided surgery that uses computed tomography, magnetic resonance imaging and stereotactic localization.
In 1970, in the city of Buenos Aires, Argentina, Aparatos Especiales company, produced the first Stereotactic System in Latin America. Antonio Martos Calvo, together with Jorge Candia and Jorge Olivetti through the request of neurosurgeon Jorge Schvarc (1942-2019), developed an equipment based on the principle of Hitchcock Stereotactic System. The patient was seated in an adapted chair with two telescopic arms attached at it base, which fixed the stereotactic frame preventing the patient’s movement.
A double radiopaque ruler attached to the side of the frame made it possible to obtain the antero-posterior and latero-lateral X-ray images without the need of moving the radiopaque ruler. The thermal coagulation lesion was performed using tungsten monopole electrodes of 1,5mm of diameter (without temperature control) with a 3mm active tip, utilizing an electrical bipolar coagulator. The lesion size was previously determined by testing the electrode in egg albumin. Coagulation size was the result of the electrical coagulator power regulation and the application time of the radiofrequency. The first surgery performed with this system was a Trigeminal Nucleotractothomy. Jorge Schvarcz performed more than 700 functional surgeries until 1994 when, due to health problems he stopped exercising his profession. But the equipment developed kept improving on a neurosurgery history.
This was the beginning of the developing of technology to produce stereotactic devices in Latin America. This was the beginning of the first stereotactic manufacturer of Latin America – The Brazilian Micromar.
Research[edit]
Stereotactic surgery is sometimes used to aid in several different types of animal research studies. Specifically, it is used to target specific sites of the brain and directly introduce pharmacological agents to the brain which otherwise may not be able to cross the blood–brain barrier.[53] In rodents, the main applications of stereotactic surgery are to introduce fluids directly to the brain or to implant cannulae and microdialysis probes. Site specific central microinjections are used when rodents do not need to be awake and behaving or when the substance to be injected has a long duration of action. For protocols in which rodents’ behaviors must be assessed soon after injection, stereotactic surgery can be used to implant a cannula through which the animal can be injected after recovery from the surgery. These protocols take longer than site-specific central injections in anesthetized mice because they require the construction of cannulae, wire plugs, and injection needles, but induce less stress in the animals because they allow for a recovery period for the healing of trauma induced to the brain before injection.[54] Surgery can also be used for microdialysis protocols to implant and tether the dialysis probe and guide cannula.[55]


