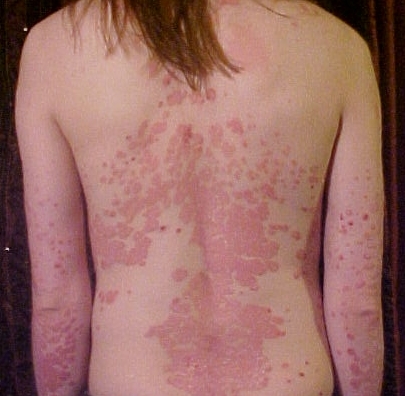
Psoriasis
Psoriasis is a long-lasting, noncontagious autoimmune disease characterized by patches of abnormal skin.[4][5] These areas are red, pink, or purple, dry, itchy, and scaly.[8][3] Psoriasis varies in severity from small localized patches to complete body coverage.[3] Injury to the skin can trigger psoriatic skin changes at that spot, which is known as the Koebner phenomenon.[9]
Psoriasis
Dermatology (primarily);
immunology, rheumatology and other specialties (e.g., cardiology and vascular medicine, nephrology, hepatology/gastroenterology, endocrinology, haematology) (indirectly/by association)
Adulthood[5]
Long-term[4]
Genetic disease triggered by environmental factors[3]
Based on symptoms[4]
Steroid creams, vitamin D3 cream, ultraviolet light, immunosuppressive drugs such as methotrexate and biologics[5]
The five main types of psoriasis are plaque, guttate, inverse, pustular, and erythrodermic.[5] Plaque psoriasis, also known as psoriasis vulgaris, makes up about 90% of cases.[4] It typically presents as red patches with white scales on top.[4] Areas of the body most commonly affected are the back of the forearms, shins, navel area, and scalp.[4] Guttate psoriasis has drop-shaped lesions.[5] Pustular psoriasis presents as small, noninfectious, pus-filled blisters.[10] Inverse psoriasis forms red patches in skin folds.[5] Erythrodermic psoriasis occurs when the rash becomes very widespread, and can develop from any of the other types.[4] Fingernails and toenails are affected in most people with psoriasis at some point in time.[4] This may include pits in the nails or changes in nail color.[4]
Psoriasis is generally thought to be a genetic disease that is triggered by environmental factors.[3] If one twin has psoriasis, the other twin is three times more likely to be affected if the twins are identical than if they are nonidentical.[4] This suggests that genetic factors predispose to psoriasis.[4] Symptoms often worsen during winter and with certain medications, such as beta blockers or NSAIDs.[4] Infections and psychological stress can also play a role.[3][5] The underlying mechanism involves the immune system reacting to skin cells.[4] Diagnosis is typically based on the signs and symptoms.[4]
There is no known cure for psoriasis, but various treatments can help control the symptoms.[4] These treatments include steroid creams, vitamin D3 cream, ultraviolet light, immunosuppressive drugs, such as methotrexate, and biologic therapies targeting specific immunologic pathways.[5] About 75% of skin involvement improves with creams alone.[4] The disease affects 2–4% of the population.[7] Men and women are affected with equal frequency.[5] The disease may begin at any age, but typically starts in adulthood.[5] Psoriasis is associated with an increased risk of psoriatic arthritis, lymphomas, cardiovascular disease, Crohn's disease, and depression.[4] Psoriatic arthritis affects up to 30% of individuals with psoriasis.[10]
The word "psoriasis" is from Greek ψωρίασις, meaning "itching condition" or "being itchy"[11] from psora, "itch", and -iasis, "action, condition".
Pathophysiology[edit]
Psoriasis is characterized by an abnormally excessive and rapid growth of the epidermal layer of the skin.[51] Abnormal production of skin cells (especially during wound repair) and an overabundance of skin cells result from the sequence of pathological events in psoriasis.[16] The sequence of pathological events in psoriasis is thought to start with an initiation phase in which an event (skin trauma, infection, or drugs) leads to activation of the immune system and then the maintenance phase consisting of chronic progression of the disease.[37][17] Skin cells are replaced every 3–5 days in psoriasis rather than the usual 28–30 days.[52] These changes are believed to stem from the premature maturation of keratinocytes induced by an inflammatory cascade in the dermis involving dendritic cells, macrophages, and T cells (three subtypes of white blood cells).[12][44] These immune cells move from the dermis to the epidermis and secrete inflammatory chemical signals (cytokines) such as interleukin-36γ, tumor necrosis factor-α, interleukin-1β, interleukin-6, and interleukin-22.[37][53] These secreted inflammatory signals are believed to stimulate keratinocytes to proliferate.[37] One hypothesis is that psoriasis involves a defect in regulatory T cells, and in the regulatory cytokine interleukin-10.[37] The inflammatory cytokines found in psoriatic nails and joints (in the case of psoriatic arthritis) are similar to those of psoriatic skin lesions, suggesting a common inflammatory mechanism.[17]
Gene mutations of proteins involved in the skin's ability to function as a barrier have been identified as markers of susceptibility for the development of psoriasis.[54][55]
Deoxyribonucleic acid (DNA) released from dying cells acts as an inflammatory stimulus in psoriasis[56] and stimulates the receptors on certain dendritic cells, which in turn produce the cytokine interferon-α.[56] In response to these chemical messages from dendritic cells and T cells, keratinocytes also secrete cytokines such as interleukin-1, interleukin-6, and tumor necrosis factor-α, which signal downstream inflammatory cells to arrive and stimulate additional inflammation.[37]
Dendritic cells bridge the innate immune system and adaptive immune system. They are increased in psoriatic lesions[51] and induce the proliferation of T cells and type 1 helper T cells (Th1). Targeted immunotherapy, as well as psoralen and ultraviolet A (PUVA) therapy, can reduce the number of dendritic cells and favors a T22 cell cytokine secretion pattern over a Th1/Th17 cell cytokine profile.[37][46] Psoriatic T cells move from the dermis into the epidermis and secrete interferon-γ and interleukin-17.[57] Interleukin-23 is known to induce the production of interleukin-17 and interleukin-22.[51][57] Interleukin-22 works in combination with interleukin-17 to induce keratinocytes to secrete neutrophil-attracting cytokines.[57]
Epidemiology[edit]
Psoriasis is estimated to affect 2–4% of the population of the western world.[7] The rate of psoriasis varies according to age, region and ethnicity; a combination of environmental and genetic factors is thought to be responsible for these differences.[7] Psoriasis is about five times more common in people of European descent than in people of Asian descent,[130] more common in countries farther from the equator,[49] relatively uncommon in African Americans, and extremely uncommon in Native Americans.[50] Psoriasis has been estimated to affect about 6.7 million Americans.[5]
Psoriasis can occur at any age, although it is more frequent in adults and commonly appears for the first time between the ages of 15 and 25 years.[5] Approximately one third of people with psoriasis report being diagnosed before age 20.[131] Psoriasis affects both sexes equally.[63]
People with inflammatory bowel disease such as Crohn disease or ulcerative colitis are at an increased risk of developing psoriasis.[49]
History[edit]
Scholars believe psoriasis to have been included among the various skin conditions called tzaraath (translated as leprosy) in the Hebrew Bible. The person was deemed "impure" (see tumah and taharah) during their affected phase and is ultimately treated by the kohen.[132] However, it is more likely that this confusion arose from the use of the same Greek term for both conditions. The Greeks used the term lepra (λέπρα) for scaly skin conditions. They used the term psora (ψώρα) to describe itchy skin conditions.[132] It became known as Willan's lepra in the late 18th century when English dermatologists Robert Willan and Thomas Bateman differentiated it from other skin diseases. Leprosy, they said, is distinguished by the regular, circular form of patches, while psoriasis is always irregular. Willan identified two categories: leprosa graecorum and psora leprosa.[133]
Psoriasis is thought to have first been described in Ancient Rome by Cornelius Celsus.[134] The British dermatologist Thomas Bateman described a possible link between psoriasis and arthritic symptoms in 1813.[134] Admiral William Halsey missed out on the Battle of Midway because he contracted psoriasis while out at sea in the early months of American participation of World War II. Admiral Chester Nimitz medically ordered Halsey to recover at a hospital in Hawaii.
The history of psoriasis is littered with treatments of dubious effectiveness and high toxicity. In the 18th and 19th centuries, Fowler's solution, which contains a poisonous and carcinogenic arsenic compound, was used by dermatologists as a treatment for psoriasis.[132] Mercury was also used for psoriasis treatment during this time period.[132] Sulfur, iodine, and phenol were also commonly used treatments for psoriasis during this era when it was incorrectly believed that psoriasis was an infectious disease.[132] Coal tars were widely used with ultraviolet light irradiation as a topical treatment approach in the early 1900s.[132][135] During the same time period, psoriatic arthritis cases were treated with intravenously administered gold preparations in the same manner as rheumatoid arthritis.[135]
Research[edit]
The role of insulin resistance in the pathogenesis of psoriasis is under investigation. Preliminary research has suggested that antioxidants such as polyphenols may have beneficial effects on the inflammation characteristic of psoriasis.[138]
Many novel medications being researched during the 2010s target the Th17/IL-23 axis,[138] particularly IL-23p19 inhibitors, as IL-23p19 is present in increased concentrations in psoriasis skin lesions while contributing less to protection against opportunistic infections.[139] Other cytokines such as IL-17 and IL-22 also have been targets for inhibition as they play important roles in the pathogenesis of psoriasis.[139] Another avenue of research has focused on the use of vascular endothelial growth factor inhibitors to treat psoriasis.[65] Oral agents being investigated during the 2010s as alternatives to medications administered by injection include Janus kinase inhibitors, protein kinase C inhibitors, mitogen-activated protein kinase inhibitors, and phosphodiesterase 4 inhibitors, all of which have proven effective in various phase 2 and 3 clinical trials.[138][139] These agents have potentially severe side-effects due to their immunosuppressive mechanisms.[139]


