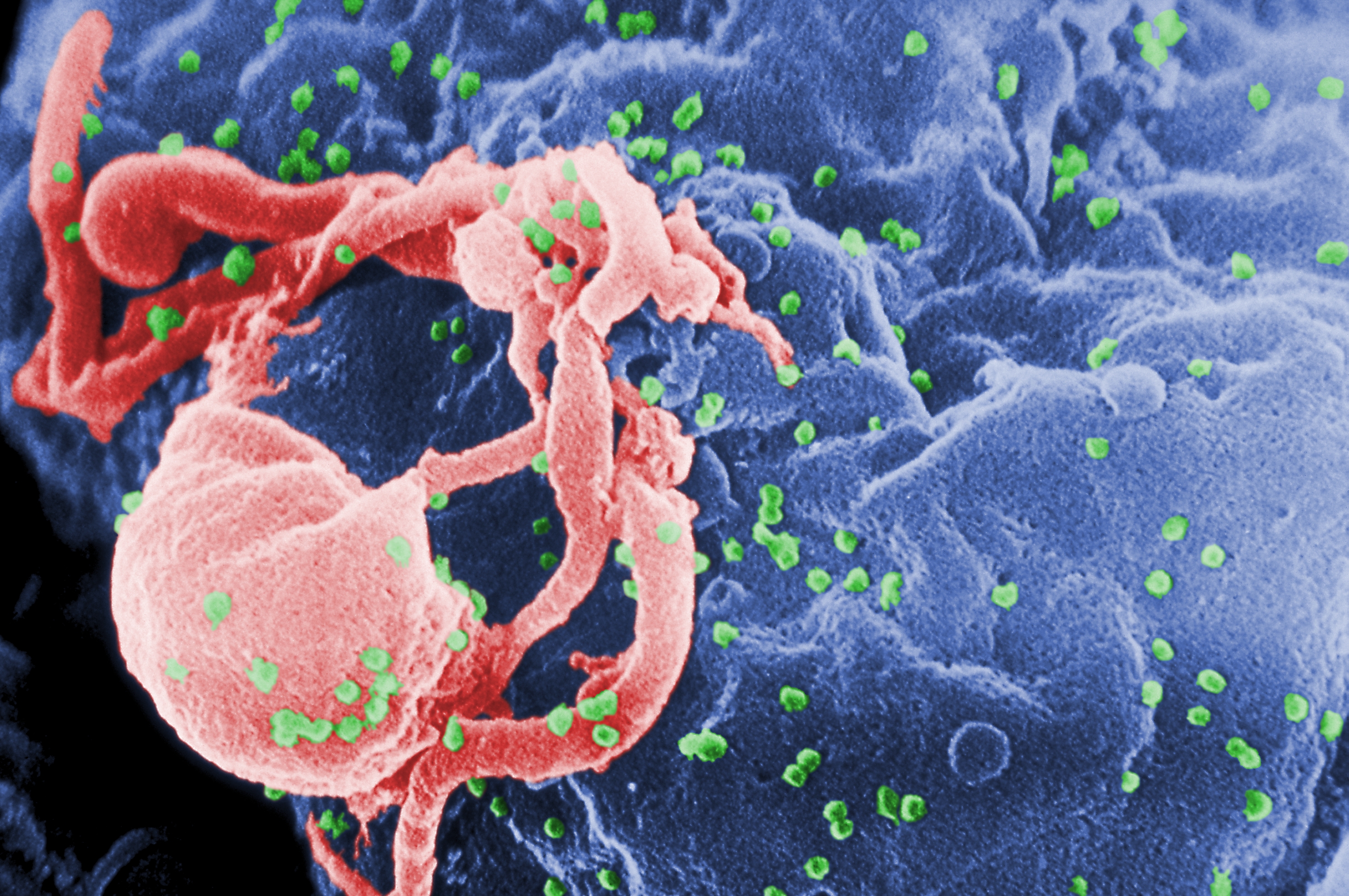
History of HIV/AIDS
AIDS is caused by a human immunodeficiency virus (HIV), which originated in non-human primates in Central and West Africa. While various sub-groups of the virus acquired human infectivity at different times, the present pandemic had its origins in the emergence of one specific strain – HIV-1 subgroup M – in Léopoldville in the Belgian Congo (now Kinshasa in the Democratic Republic of the Congo) in the 1920s.[1]
There are two types of HIV: HIV-1 and HIV-2. HIV-1 is more virulent, more easily transmitted, and it is the cause of the vast majority of HIV infections globally.[2] The pandemic strain of HIV-1 is closely related to a virus found in chimpanzees of the subspecies Pan troglodytes troglodytes, which live in the forests of the Central African nations of Cameroon, Equatorial Guinea, Gabon, the Republic of the Congo, and the Central African Republic. HIV-2 is less transmissible and is largely confined to West Africa, along with its closest relative, a virus of the sooty mangabey (Cercocebus atys atys), an Old World monkey inhabiting southern Senegal, Guinea-Bissau, Guinea, Sierra Leone, Liberia, and western Ivory Coast.[2][3]
Emergence[edit]
Unresolved questions about HIV origins and emergence[edit]
The discovery of the main HIV/SIV phylogenetic relationships permits explaining broad HIV biogeography: the early centres of the HIV-1 groups were in Central Africa, where the primate reservoirs of the related SIVcpz and SIVgor viruses (chimpanzees and gorillas) exist; similarly, the HIV-2 groups had their centres in West Africa, where sooty mangabeys, which harbour the related SIVsmm virus, exist. However, these relationships do not explain more detailed patterns of biogeography, such as why epidemic HIV-2 groups (A and B) only evolved in the Ivory Coast, which is one of only six countries harbouring the sooty mangabey. It is also unclear why the SIVcpz endemic in the chimpanzee subspecies Pan troglodytes schweinfurthii (inhabiting the Democratic Republic of Congo, Central African Republic, Rwanda, Burundi, Uganda, and Tanzania) did not spawn an epidemic HIV-1 strain to humans, while the Democratic Republic of Congo was the main centre of HIV-1 group M, a virus descended from SIVcpz strains of a subspecies (Pan troglodytes troglodytes) that does not exist in this country. It is clear that the several HIV-1 and HIV-2 strains descend from SIVcpz, SIVgor, and SIVsmm viruses,[3][8][9][10][12][20] and that bushmeat practice provides the most plausible cause of cross-species transfer to humans.[10][12][25] However, some loose ends remain.
It is not yet explained why only four HIV groups (HIV-1 groups M and O, and HIV-2 groups A and B) spread considerably in human populations, despite bushmeat practices being widespread in Central and West Africa,[13] and the resulting human SIV infections being common.[25]
It also remains unexplained why all epidemic HIV groups emerged in humans nearly simultaneously, and only in the 20th century, despite very old human exposure to SIV (a 2010 phylogenetic study demonstrated that SIV is at least tens of thousands of years old).[26]
Origin and epidemic emergence[edit]
Several of the theories of HIV origin accept the established knowledge of the HIV/SIV phylogenetic relationships, and also accept that bushmeat practice was the most likely cause of the initial transfer to humans. All of them propose that the simultaneous epidemic emergences of four HIV groups in the late 19th-early 20th century, and the lack of previous known emergences, are explained by new factor(s) that appeared in the relevant African regions in that timeframe. These new factor(s) would have acted either to increase human exposures to SIV, to help it to adapt to the human organism by mutation (thus enhancing its between-humans transmissibility), or to cause an initial burst of transmissions crossing an epidemiological threshold, and therefore increasing the probability of continued spread.
Genetic studies of the virus suggested in 2008 that the most recent common ancestor of the HIV-1 M group dates back to the Belgian Congo city of Léopoldville (modern Kinshasa), circa 1910.[17] Proponents of this dating link the HIV epidemic with the emergence of colonialism and growth of large colonial African cities, leading to social changes, including a higher degree of non-monogamous sexual activity, the spread of prostitution, and the concomitant high frequency of genital ulcer diseases (such as syphilis) in nascent colonial cities.[13]
In 2014, a study conducted by scientists from the University of Oxford and the University of Leuven, in Belgium, revealed that because approximately one million people every year would flow through the prominent city of Kinshasa,[1] which served as the origin of the first known HIV cases in the 1920s,[1] passengers riding on the region's Belgian railway trains were able to spread the virus to larger areas.[1] The study also identified a roaring sex trade, rapid population growth and unsterilised needles used in health clinics as other factors which contributed to the emergence of the Africa HIV epidemic.[1]
Pathogenicity of SIV in non-human primates[edit]
In most non-human primate species, natural SIV infection does not cause a fatal disease (but see below). Comparison of the gene sequence of SIV with HIV should, therefore, provide information about the factors necessary to cause disease in humans. The factors that determine the virulence of HIV as compared to most SIVs are only now being elucidated. Non-human SIVs contain a nef gene that down-regulates CD3, CD4, and MHC class I expression; most non-human SIVs, therefore, do not induce immunodeficiency; the HIV-1 nef gene, however, has lost its ability to down-regulate CD3, which results in the immune activation and apoptosis that is characteristic of chronic HIV infection.[45]
In addition, a long-term survey of chimpanzees naturally infected with SIVcpz in Gombe National Park, Tanzania found that, contrary to the previous paradigm, chimpanzees with SIVcpz infection do experience an increased mortality, and also suffer from a human AIDS-like illness.[46] SIV pathogenicity in wild animals could exist in other chimpanzee subspecies and other primate species as well, and stay unrecognized by lack of relevant long term studies.
Activism by AIDS patients and families[edit]
During the beginning of the HIV/AIDS epidemic, it was believed that this disease mainly affected gay, white males. Due to this misconception, people of colour were provided with no information or services in order to educate and help those who were HIV positive. Fortunately, as more activists spoke out about their concerns, organizations, such as Black Coalition For AIDS Prevention and Alliance For South Asian AIDS Prevention came to be, providing their communities with services in order to enhance the lives of HIV positive individuals and to reduce the spread of HIV/AIDS. [101]
In New York City, Nathan Fain, Larry Kramer, Larry Mass, Paul Popham, Paul Rapoport, and Edmund White officially established the Gay Men's Health Crisis (GMHC) in 1982.[102][103][104]
Also in 1982, Michael Callen and Richard Berkowitz published How to Have Sex in an Epidemic: One Approach. In this short work, they described ways gay men could be sexual and affectionate while dramatically reducing the risk of contracting or spreading HIV. Both authors were themselves gay men living with AIDS. This booklet was one of the first times men were advised to use condoms when having sexual relations with other men.[105]
At the beginning of the AIDS epidemic in the 1980s, there was very little information about the disease. Because AIDS disproportionately affected stigmatized groups, such as homosexuals, people of low socioeconomic status, sex workers and addicts, there was also initially little mass media coverage when the epidemic started.[106] However, with the rise of activist groups composed of people suffering from AIDS, either directly or through a loved one, more public attention was brought to the epidemic.[107]
Identification of the virus[edit]
May 1983: LAV[edit]
In May 1983, a team of doctors at the Pasteur Institute in France including Françoise Barré-Sinoussi and Luc Montagnier reported that they had isolated a new retrovirus from lymphoid ganglions that they believed was the cause of AIDS.[108] The virus was later named lymphadenopathy-associated virus (LAV) and a sample was sent to the U.S. Centers for Disease Control, which was later passed to the National Cancer Institute (NCI).[108][109]
May 1984: HTLV-III[edit]
In May 1984 a team led by Robert Gallo of the United States confirmed the discovery of the virus, but they renamed it human T lymphotropic virus type III (HTLV-III).[110]
January 1985: both found to be the same[edit]
In January 1985, a number of more-detailed reports were published concerning LAV and HTLV-III, and by March it was clear that the viruses were the same—indeed, it was later determined that the virus isolated by the Gallo lab was from the lymph nodes of the patient studied in the original 1983 report by Montagnier[112]—and was the etiological agent of AIDS.[113][114]
May 1986: the name HIV[edit]
In May 1986, the International Committee on Taxonomy of Viruses ruled that both names should be dropped and a new name, HIV (Human Immunodeficiency Virus), be used.[115]
Nobel[edit]
Whether Barré-Sinoussi and Montagnier deserve more credit than Gallo for the discovery of the virus that causes AIDS has been a matter of considerable controversy. Barré-Sinoussi and Montagnier were awarded the 2008 Nobel Prize in Physiology or Medicine for their "discovery of human immunodeficiency virus",[116] and Harald zur Hausen also shared the prize for his discovery that human papilloma virus leads to cervical cancer, but Gallo was left out.[117] Gallo said that it was "a disappointment" that he was not named a co-recipient.[118] Montagnier said he was "surprised" Gallo was not recognized by the Nobel Committee: "It was important to prove that HIV was the cause of AIDS, and Gallo had a very important role in that. I'm very sorry for Robert Gallo."[117] Dr Levy's contribution to the discovery of HIV was also cited in the Nobel Prize ceremony.
Case definition for epidemiological surveillance[edit]
Since June 5, 1981, many definitions have been developed for epidemiological surveillance such as the Bangui definition and the 1994 expanded World Health Organization AIDS case definition.